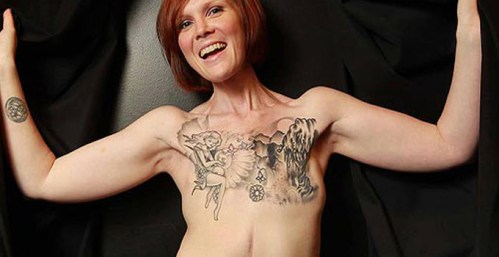
Fear is one of my constant companions on this cancer journey, for nearly four years now it has attempted to overcome me and prevent me from living the life I want. Naturally, when I was first diagnosed with ovarian cancer and saw my pathology report a series of unsettling questions raced through my mind. Consulting with a team of oncologists at Calgary’s Baker Centre only seemed to increase my anxiety over my condition. Will the recommended treatment be successful or will I die? Will undergoing another major surgery followed by chemotherapy be too agonizing and unbearable? Now that my oncologist has informed me that I’m in remission, it’s the fear of my cancer recurring that I have to cope with on a daily basis.
In this post I’d like to share several of the best techniques that I’ve discovered for cancer survivors to master their fear and not let it control them.
Remember That Your Journey is Unique
Most women with ovarian cancer have at least one relapse within five years of being diagnosed, but I frequently remind myself that this standard rate of recurrence won’t necessary happen to me. The reality is that medical science has established that all cancer patients are unique. What’s more, because cancer statistics are based on large samples of people, they cannot be used to predict exactly what will happen to a single individual. Everyone is different. Treatments and how people respond to treatment can differ greatly. I strongly suggest trying to follow these essential rules:
- Resist the temptation to compare the disease in your body to what is happening to other people, even in situations when the type or stage of cancer is highly similar.
- Don’t dwell on statistics or the possibility of recurrence.
Practice Mindfulness
I’ve discovered that one of the best ways to quiet my mind and focus my attention is a technique called mindfulness. Jon Kabat-Zinn pioneered using this method with cancer patients and other groups battling chronic pain or illness at the University of Massachusetts Medical School. Mindfulness is basically just a way of paying attention, a way of awakening our minds and being present in the here and now. With principles found in Buddhism, mindfulness teaches us to live moments in each day rather than focusing on what might lie ahead.
Acceptance and letting go are crucial components of mindfulness. A philosophy of mindfulness encourages us to come to terms with our life, even difficult experiences such as a cancer diagnosis. Acceptance means seeing things as they actually are in the present. Mindfulness doesn’t require that you have to like your situation—you don’t necessarily have to assume a passive attitude toward suffering or life’s unfairness. However, you must come to terms with things as they are and acknowledge them, whether it’s a diagnosis of cancer or the possibility of its recurrence in the future.
Appreciate the Joys of Nature
It’s generally agreed that exposure to nature is extremely beneficial for people with cancer or other chronic illnesses, improving mood and easing anxiety, stress, and depression. Current research findings suggest that natural settings such as parks, wilderness areas, urban green spaces and gardens have the potential to improve both physical and mental health. Numerous health scholars claim that ecotherapy can promote wellness and healing. The practice is also known as green therapy, nature therapy, and earth-centered therapy.
Take Part in Exercise or Physical Activity
Studies have proven the benefits of exercise for cancer patients. Of course, vigorous physical activity might not be possible during treatment and you should always consult with your doctor before beginning an exercise program. It will take more effort to become active if you were accustomed to a sedentary lifestyle before your cancer diagnosis. Many people feel so excited about “getting healthy” that they try to do multiple things at once, and that’s a recipe for burnout. Try focusing on just one type of exercise first. Some research indicates that a behavior change is more likely to ensue when you’ve identified what you really want from it. You may be seeking better moods or stress relief, or maybe you just want to connect with a fellow cancer survivor or workout buddy—it doesn’t matter, as long as you know what your goals are.
Have at Least One Regular Hobby

There’s an emerging group of professionals who employ the arts to help people heal. The new field is called creative arts therapies, and it encompasses a wide range of modes of expression including art, dance/movement, drama, music and poetry. When cancer patients undertake these activities, whether individually or with the guidance of a creative art therapist, they stand to benefit psychologically and emotionally. Recently there’s been a trend toward simple or old-fashioned crafts and hobbies such as knitting. Some adults are even using colouring books to relax and reduce daily stress. This concept started several years ago with the publication of Johanna Basford’s Secret Garden. Her colouring book for adults has since been translated into 14 languages and has sold over one million copies.