Only recently have I started to think a great deal about the history of cancer or the oncologists and patients that have come before me. I developed a fascination with these topics while watching the PBS miniseries Cancer: The Emperor of All Maladies. This three part series skillfully explores the medical and scientific aspects of cancer; even more impressive is the wonderful job that the producers have done of delving into its history and politics.
Only recently have I started to think a great deal about the history of cancer or the oncologists and patients that have come before me. I developed a fascination with these topics while watching the PBS miniseries Cancer: The Emperor of All Maladies. This three part series skillfully explores the medical and scientific aspects of cancer; even more impressive is the wonderful job that the producers have done of delving into its history and politics.
The creators of the groundbreaking television documentary based their project on a strong work of non-fiction by renowned oncologist and award winning journalist Siddhartha Mukherjee. Both the PBS documentary and Mukherjee’s Pulitzer Prize winning volume have one overriding theme. They bring to light that our current generation’s experience with cancer represents only a momentary chapter in an epic battle spanning thousands of years.
The Emergence of Modern Cancer Surgery
When I was diagnosed with fairly advanced cancer in my uterus and right ovary, the first, and most essential, part of my medical treatment involved surgery. I literally owe my life to the skill of my pelvic cancer surgeons and to the sophisticated surgical techniques available in the 21st century. Ovarian cancer is still the most serious of all women’s cancers, and the survival rates can be quite grim—the positive news is that the outlook has improved in recent decades, largely due to better surgical procedures.
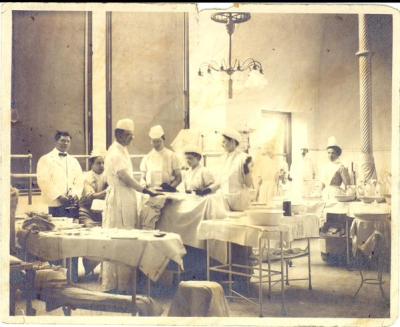
For centuries surgery to remove cancerous tumours wasn’t a viable option, as the medical technology wasn’t yet available. In extremely rare cases a physician would attempt to cut out a cancerous growth. However, the circumstances would have been barbaric by today’s standards. There was no method to properly anesthetize patients and they were frequently operated on while conscious, in addition there was no use of modern antiseptics to keep the surgical wounds from becoming infected.
The late 19th century witnessed the origins of present-day cancer surgery. Anesthetics such as either were discovered and this made lengthier, more complex operations possible. Procedures such as the radical mastectomy for breast cancer were successfully devised and implemented during this era. As a matter of fact, the medical community firmly believed that it was possible to cure cancer through surgery alone. The nature of how cancer spreads to distant sites in the body wasn’t yet well understood. Most experts mistakenly believed that its recurrence months or years after surgery was strictly due to not taking out enough tissue, reappearance of the disease was caused by the growth of fragments of the principle tumour that were left behind.
The Development of Chemotherapy
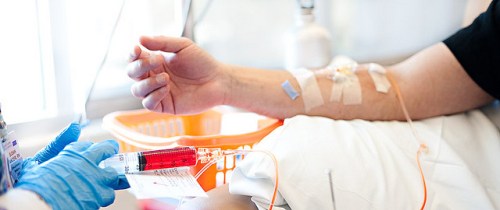
The nature of metastasis is much better understood today and a patient with gynecological cancer, such as myself, is routinely offered chemotherapy following surgery. Of course only in the past 40 or 50 years have powerful chemotherapy drugs been introduced to the arsenal in the war against cancer. Oncologist Sidney Farber (1903-1973) is considered by most historians to be the father of chemotherapy. Farber and his team in Boston began trials on children with leukemia in the late 1940s. At this time leukemia was still a death sentence for any child diagnosed with the disease.
Farber’s new therapy was almost miraculous in the sense that it led to remission in many of his young patients. Some of the children, including a patient named Robert Sandler, had their lives extended by months after the potent chemicals were administered to them. The leukemia would virtually disappear and they would momentarily resume an active childhood. Throughout the 1950s and 60s, Farber continued to make advances in cancer research, notably the 1955 discovery that the antibiotic actinomycin D and radiation therapy could produce remission in Wilms’ tumor, a pediatric cancer of the kidneys.
What the Future Holds
As I battle ovarian cancer I try to be realistic about how far treatment has come, I know there is still an extremely long way to go in the war against this insidious disease. Over the last two decades, the five-year survival rate for patients with ovarian cancer has improved significantly. Yet, according to the experts, no more than 30 per cent of long-term ovarian cancers are currently being cured. Oncologists admit that they are facing enormous challenges. While surgical advances and new treatment approvals, including Lynparza (olaparib) and Avastin (bevacizumab), have improved the outlook for ovarian cancer patients, late diagnosis and tumour resistance remain as the two most significant barriers in overcoming the disease.
Meanwhile, the medical community is continuously developing new treatments for cancer, one of the most promising is called immunotherapy. For decades oncologists have known that the immune system plays an important role in certain types of cancer. They noted that there were rare spontaneous remissions of cancer without treatment and they suspected that this was because the immune system was attacking the tumour. Immunotherapy is designed to boost the body’s natural defenses to fight the cancer. Medical specialists use materials either made by the body or in a laboratory to improve, target, or restore immune system function.
At the present time it isn’t entirely clear how immunotherapy works against cancer, it may function by stopping or slowing the growth of cancer cells, stopping cancer from spreading to other parts of the body, or helping the immune system increase its effectiveness at eliminating cancer cells. There are currently several types of immunotherapy in use, including monoclonal antibodies, non-specific immunotherapies, and cancer vaccines.