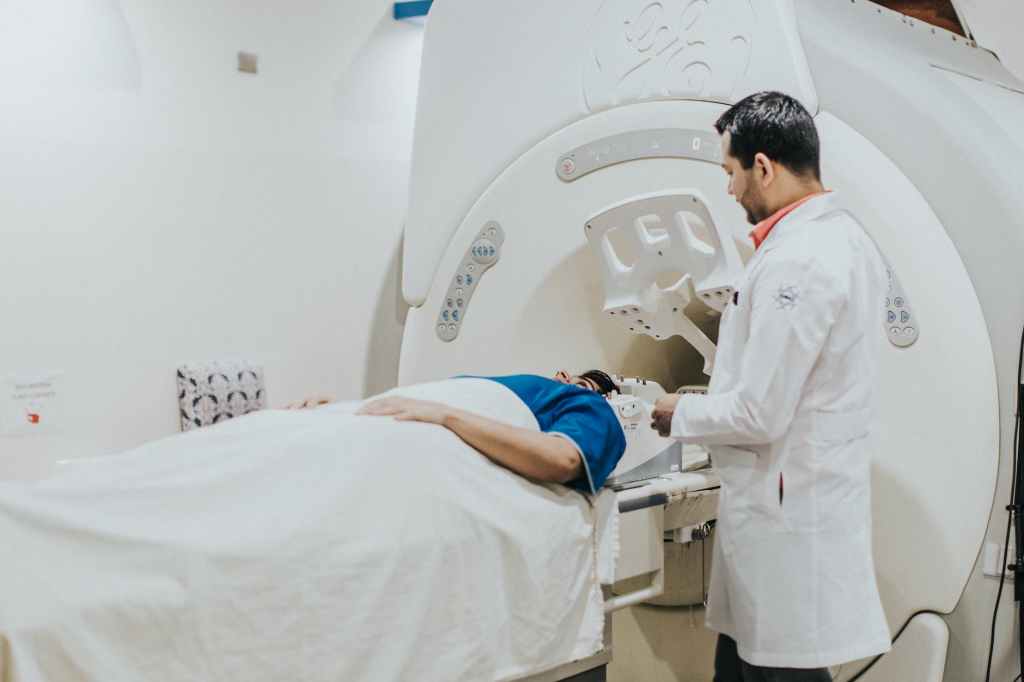
I underwent several major surgeries as well as chemotherapy for my ovarian cancer approximately a decade ago, meanwhile I watch in amazement as I observe many of the new options that are available for patients today. In my opinion the speed at which cancer treatment and patient care have evolved is truly amazing.
One perfect example is that today many patients who are diagnosed with cancer are assigned a nurse navigator through their cancer centre. When I was going through treatment, I didn’t have access to one because at that time nurse navigators were still extremely rare. I believe that if I’d been matched with a nurse to work with me one on one, it would have made my adjustment to becoming a cancer patient less stressful and a great deal easier.
What exactly is a nurse navigator and how do they assist you when you’re going through one of the most confusing and turbulent periods of your life? Nurse navigators are now commonly employed in oncology to help patients through their cancer diagnosis and individualized care plan. An oncology nurse navigator (ONN) is usually a professional registered nurse with oncology-specific clinical knowledge. Their job is to offer individualized assistance to patients, families, and caregivers. Essentially a navigator is there to help you overcome healthcare system barriers. In essence your navigator is your advocate for care—from initial consultation right through treatment.
The CBC radio show White Coat Black Art recently covered the topic of nurse navigators. The first cancer navigation program in Canada was created in 2002 in Nova Scotia, followed by Quebec launching a similar program in 2005. Most provinces and territories have since implemented different forms of a cancer navigation program. Programs between provinces differ — from who is covered, to what a navigator helps with. Each health authority has adopted a distinct strategy and customized the program for their region.
Lorie Kielley is a registered nurse who works as a cancer patient navigator with Newfoundland and Labrador Health Services. “Having someone to reach out to, to guide them through what to expect, what supports are available to them and guide them through the whole process, is definitely something that can at least take a little bit of stress out of the experience,” Kielley told White Coat.
I’m grateful that if I must go through cancer treatment again, I’ll be much more likely to reap the benefits of my own personal nurse navigator. There are other important innovations that I’m aware of at my cancer centre —for one thing, Enhanced Recovery After Surgery (ERAS) frequently makes surgery less difficult for patients. Drawing from best practices and evidence from around the world, this new approach improves patient care related to nutrition, mobility after surgery, fluid management, anesthesia, and pain control.
When I underwent surgery there were some standard protocols that I found hard to bear and that probably made my body even more weak when I was struggling to recover. First, I was required to fast for 48 hours and prepare my bowel by drinking noxious medications, then I was taken shivering into a cold operating room. This isn’t the case with some gynecologic cancer patients today, some women at my cancer centre are able to participate in ERAS. On the day of their surgery, they’re usually allowed to drink or eat until just a few hours before their procedure and they’re kept warm and comfortable, even after they enter the operating room.
Instead of rigorous fasting and becoming stressed out in the days or weeks leading up to my surgery ERAS would recommend enhanced nutrition and physical activity to make sure that I was in optimum condition for a major surgical procedure. This new method makes patients part of the team by involving them in preparation for their surgery and post-operative recovery. The main objective is to help patients stay strong, improve outcomes, and reduce complications.
ERAS guidelines consist of about 20 different practices before, during and after surgery. They include keeping patients well-nourished, giving them anti-coagulants and pre-operative antibiotics, avoiding cold in the operating room, avoiding the use of long-acting sedatives, using non-opioid pain medications (where alternatives are medically appropriate), using anti-nauseants, and encouraging patients to move as soon as possible after surgery.
Meanwhile, my standard surgical recovery was almost gruelling, I needed to be hospitalized for 10 days before I was finally released. The encouraging news is that at my cancer centre there are now some patients who would normally spend about 10 days recovering from surgery going home in only five days because of ERAS. “Everything just went so smoothly, there was no reason for me to hang around,” one patient recalls. “I felt great — the nausea was well-controlled, the pain was well-controlled, and I was up and walking. It was incredible — you don’t want to stay in hospital any longer than you need to.”
Despite recent progress, I still try to be realistic about how far treatment for ovarian cancer has come, I know there’s still an extremely long way to go in the war against this insidious disease. Ovarian cancer patients are having better outcomes because they have more treatment options, but the cancer still frustrates doctors and their patients because it often remains undetected until it has spread. Oncologists admit that they are facing enormous challenges. While surgical advances and new treatment approvals have improved the outlook for ovarian cancer patients, late diagnosis and tumour resistance remain as the two most significant barriers in overcoming the disease.